Severe knee pain means there is a joint problem. The peculiarity of the knee joint is that it takes the main load during movement and physical exertion, due to which it is often injured. The affected knee is difficult to fix, so it is very important to take measures to promptly eliminate the cause of pain.
Main reasons
The causes of knee pain can be:
- Injuries (acute injuries).They are the most common cause. They occur after a strong blow, excessive bending of the joint and a sharp fall on it. In mechanical injury there is sharp pain, swelling, there may be a tingling sensation, tingling, skin color in the joints changes.
- arthrosis (gonarthrosis)is the destruction of joint tissues. Gonarthrosis is primary and secondary. The primary disease affects the elderly, while the secondary causes the consequences of injuries or is a complication of other diseases (eg rheumatoid arthritis). Symptoms: pain and stiffness in the joint. With a long course of gonarthrosis, movements in the joint may become impossible.
- arthritis- inflammatory disease. Distinctive signs: pain that increases with movement, increase in the size of the joint, fever in the affected knee, redness at times.
- Meniscopathy- damage to the meniscus, which manifests itself in acute pain. In the absence of appropriate treatment, a transition to a chronic form is possible, as a result of which osteoarthritis develops.
- Vascular diseases. Thrombosis or embolism (blockage) of the arteries that supply the knee joint leads to osteonecrosis of the articular cartilage, making walking impossible. There are no effective treatments for osteonecrosis. Arthroplasty of the affected joint is performed.
- periarthritis- This is an inflammation of the joint sac and the tissues that surround it. In periarthritis there is pain in the knee joint without a clear location. Periarthritis is most often a post-traumatic complication.
- bursitisis an inflammation of the synovial sac (bursa). Bursitis can be caused by overuse of the joint, infection or injury. In this disease there is severe constant pain, but freedom of movement is preserved.
- TendinitisThis is an inflammation of the ligaments and tendons. Symptoms include swelling and pain in the affected area. They increase with flexion-extension of the knees. Prolonged symptoms of tendinitis are indicative of tendinosis.
- Baker's cyst- this is a complication after trauma, gonarthrosis or hemarthrosis. Baker's cyst is a collection of joint fluid in the popliteal sac. The pathology is characterized by pain when bending the knee and a feeling of discomfort during movement. To avoid complications, it is strongly recommended that you do not squat.
- Osteomyelitis of the bones of the legsis a purulent disease associated with infection resulting from hematogenous osteomyelitis, an open fracture or a postoperative complication. The most common infectious agent is staphylococci.
Varieties of pain
There are such types of knee pain:
- When squatting. It is usually caused by joint disease, viral infection, lack of physical activity, poor nutrition. is observed in athletes. If your knees hurt when squatting, then the exercises should be stopped. In case of prolonged and frequent pain you should consult a doctor.
- When bending the legs. This is one of the most common joint problems. It is observed in Osgood-Schlatter's disease, damage to ligaments and meniscus, Baker's cyst, infectious lesions, etc. When pain occurs, it is necessary to limit the load on the legs, to refuse to play sports, to wear comfortable orthopedicshoes.
- After running. Related to diseases such as osteoarthritis, bursitis, synovitis and others. In this case, the normal functioning of the joint stops and under heavy loads it begins to collapse. It is necessary to carry out timely treatment of these diseases, otherwise complete loss of motor functions is possible.
- Crunching. If there is no swelling, pain and stiffness when moving, then you have nothing to fear. However, this symptom can be caused by a dangerous disease - osteoarthritis, which damages the articular cartilage and causes severe pain. It is very important to start timely treatment of this disease.
Diagnosis
You can diagnose the cause of the pain in the following ways:
- General blood test. Allows you to detect anemia, leukocytosis and more.
- Blood chemistry. Detects an increase in uric acid in gout.
- X-ray examination. This method allows you to detect bone pathology. It is used to diagnose fractures, osteomyelitis and osteoarthritis. X-rays are complemented by computed tomography (CT). Menisci, ligaments, bursae and other soft tissues are not visible on X-rays and CT scans.
- MRI (magnetic resonance imaging), MRI (magnetic resonance imaging). This is modern research. With its help the pathology of the soft tissues of the joint (menisci, ligaments, etc. ) is diagnosed.
- Puncture bone biopsy. It is performed when osteomyelitis or bone tuberculosis is suspected.
- Arthroscopy. It is performed for both diagnosis and treatment, for example in case of meniscus injury.
- Ultrasound (ultrasound examination). This is a screening study conducted in cases of suspected traumatic injuries, osteoarthritis, meniscus disease and others. Ultrasound results should be confirmed by radiography (CT) and / or MRI.
Treatment
Treatment should be comprehensive and include both conservative methods and surgery. Let's look at them in more detail:
conservative methods
During exacerbations, treatment should relieve pain and swelling and then restore normal joint mobility. For the first time after an injury, it is not recommended to move without assistance.
The basis of treatment is anti-inflammatory therapy. It includes the use of the following agents: non-steroidal anti-inflammatory drugs, pyrazolone derivatives, indoleacetic acid derivatives, oxicam, glucocorticoids.
The following procedures are prescribed to strengthen the immune system: cryopheresis, plasmapheresis, chemisorption, plasma filtration, immunostimulants.
The specific drug and method of treatment is chosen by the attending physician.
Also, conservative treatment includes ice packs on the injured area to relieve pain or hot compresses to improve blood microcirculation.
In hemarthrosis, the joint is punctured and the blood accumulated due to trauma is removed.
Also, conservative treatment includes physiotherapy methods: massage, therapeutic exercises and spa rehabilitation. If necessary, the doctor prescribes a special diet that provides a limited calorie content.
Chondroprotectors are used to nourish cartilage and reduce destructive processes.
The most common physiotherapy methods are magnetic therapy, laser therapy, cryotherapy, acupuncture.
In gonarthrosis, special shoes and knee braces are used - orthoses. These shoes contribute to the normalization of gait, and the knees fix the diseased joint.
Surgical intervention
If, after conservative treatment, it is not possible to achieve the required stability of the joint, surgery is indicated.
The most common surgical techniques are arthroscopy and arthroplasty.
Arthroscopy is a technique that can relieve joint pain and increase joint mobility. This method of treatment not only eliminates the underlying disease, but also allows you to introduce drugs into the joint cavity that reduce inflammation.
Doctor's advice
Hyaluronic acid preparations given intra-articularly have a pronounced therapeutic effect in osteoarthritis of the 2nd and even 3rd stages. The introduction of hyaluronic acid is considered an alternative to arthroplasty when it is impossible due to therapeutic contraindications. This is a medical procedure, there are contraindications.
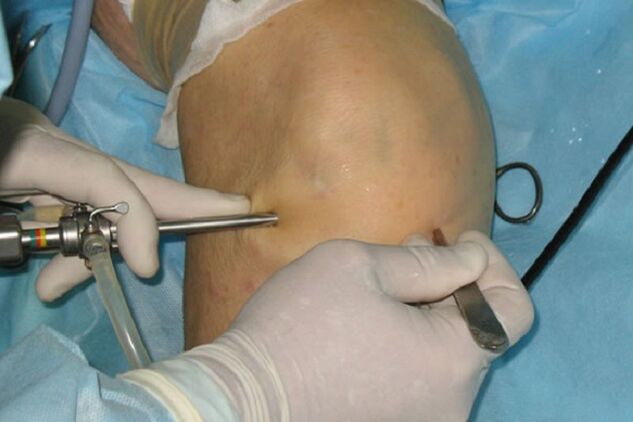
The technique is performed for such problems:
- damage to the meniscus and cartilage;
- ligament rupture;
- the presence of foreign bodies in the joint;
- rheumatoid arthritis;
- intra-articular fractures.
During the period of postoperative rehabilitation, it is recommended to strictly follow the medical recommendations, performing therapeutic exercises, avoiding unjustified early loading of the limb.
Endoprosthesis (arthroplasty) is an operation in which the damaged parts of the knee joint are replaced with an artificial implant (endoprosthesis).
More than 95% of endoprostheses, which are placed under compulsory medical insurance, function for 10-15 years, after which they must be replaced. Today, far from all regions, the replacement of an endoprosthesis, unlike the primary operation, can be issued under compulsory medical insurance. Not all patients after 10-15 years can undergo a second operation due to cardiovascular and other somatic risks. That is why it is not worth rushing to endoprosthetics. I recommend resorting to this operation only when all other treatment options are exhausted.
Endoprosthesis is performed when the restoration of painless function of the knee joint is not possible with conservative methods and with the help of arthroscopy. After arthroplasty, purulent complications are possible. Antibiotics are prescribed for their prevention. After endoprosthesis, long-term rehabilitation of the patient is required (up to 6 months).
Folk remedies
Folk remedies can be useful to relieve pain, but they should be done in parallel with conventional treatments.
When using folk remedies, be sure to consult a doctor.
Let's look at some popular methods:
- Ointment. For knee pain, prepare 1 tbsp hypericum and 2 tbsp yarrow by crushing them. Melt 1 tablespoon Vaseline in a water bath. The grass is poured into hot Vaseline and rubbed to a homogeneous mass. This ointment should be rubbed on sore knees at night.
- A mixture based on rye seeds. You need to take 250 g of rye seeds, fill them with 2 liters of water and boil. After the mixture cools, strain and add 500 g of vodka, 1 kg of honey, 3 tsp barberry root. The mixture is mixed well and left for 21 days in a dark place. It is recommended to use a mixture of 3 tablespoons before eating. For the period of treatment it is necessary to drink 9 liters of the mixture.
If you have knee pain, don't panic. However, if the pain persists for a long time, you should definitely consult a doctor. This will avoid a lot of trouble.



































